Specialized Centers
Hip Arthroscopy
The hip joint has two parts: the upper end of the femur (thighbone) called the femoral head and the acetabulum (hip socket). In a healthy hip, these components are covered with even, smooth cartilage that allows pain-free movement. If a joint is diseased, the cartilage breaks down and the patient feels pain, stiffness and loss of motion, which has a detrimental effect on quality of life.
Certain patients, especially young people and athletes, may injure the femur or acetabulum, which can damage the joint structure, such as the labrum (cartilage). If these injuries are not treated quickly they can lead to articular deterioration, which is the start of early osteoarthrosis.
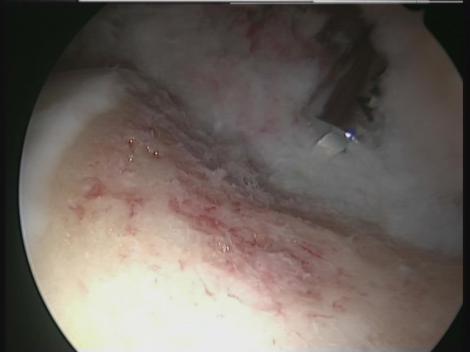
Hip arthroscopy is a recently developed technique that allows the joint injuries in the hip or its surrounding area to be treated through two or three small incisions in the skin measuring less than a centimetre.
Benefits of the Operation
This technique is used to treat hip patients who do sport or who used to do it in the past and who suffer from pain in the ground which, until now, required far more complex surgery and much longer recovery periods.
Now it is possible to relieve these patients' symptoms so they can resume their sporting activities as well as taking action to prevent early osteoarthritis of the hip.
Medical-technical description
The following hip joint problems are suitable for treatment by arthroscopy:
- Hip impingement (cam or femoro acetabular impingement): Arthroscopic techniques are used to treat bone deformities that affect either the femur (cam impingement) or the acetabulum (pincer impingement), as well as all injuries involving the joint cartilage and acetabular labrum (the fibrocartilage that runs completely around the acetabulum) during the same surgical intervention. This makes it possible to stabilise injuries which are known to cause long-term wear and tear on the joint and, consequently, osteoarthritis of the hip.
- Snapping hip syndrome (Perrin-Ferraton disease): This can be resolved with small incisions in the snapping hip, both externally (in the traochanter area) or internally, produced by the psoas muscle.
- Removal of loose bodies that may appear after a hip injury or due to degenerative arthritis, which can cause a "catching" in the joint.
- Joint infection, whatever the cause of the infection might be, can be treated satisfactorily using this innovative technique. The infection is removed by cleaning and washing out the joint.
- Diagnosis and treatment of impingement and snapping problems in patients with painful hip prostheses.
About the operation
Hip arthroscopy takes place in the operating theatre. The surgery usually takes between one and two hours, depending on the injuries to treat. The patient is in theatre and recovery room for between three and five hours. Patients usually spend a night in hospital and are able to go home the following day. On release, they are given a release report setting out the recommendations, treatment to follow and subsequent appointments.
Before the operation
- The patient goes to the doctor's office for a prior consultation, when decisions are taken and the doctor explains the surgery in detail and gives the patient an informed consent.
- You must take a list of all the medications you usually take (including medicinal plants) to the hospital with you on the day of your surgery.
- You will have pre-surgical tests consisting of a full blood test, biochemistry, coagulation, chest x-ray and ECG.
- You must wash the surgical site with an antiseptic night before and on the morning of the surgery.
- Get hold of two crutches or walking sticks you will need for the first three or four weeks after the operation.
- If you are to have your surgery in the morning, you must not eat or drink anything that morning. If the surgery is to take place in the afternoon, have an early breakfast then do not eat or drink anything after 9 am.
- You must remove all metal objects during the operation (rings, bracelets, earrings, body piercings, etc.).
Post-operative care
- You will start moving on the first day. You must not put more than 50% of your weight on the joint for the first three or four weeks, so you will need to use two crutches. In any case, you must follow the instructions you will be given by your surgeon.
- Correct rehabilitation is necessary, so on the first few days you must not travel or do any strenuous or violent movements.
- We do not recommend using the crutches while holding your leg off the floor, because this may cause abnormal healing of the hip flexion.
- After release, you should contact us if you suffer from chest pain or have breathing difficulties, swelling or reddening in a leg, sharp pain in the hip on which you have had the surgery, fever or shivering.
- On release, you will be given a set of exercises to do at home every day. After the second week we recommend you use an exercise bike for 20 to 30 minutes every day, without resistance. After three weeks we recommend you start exercising in a swimming pool.
- You will receive anti-clotting and antibiotic treatment while you are in hospital.
The importance of immediate rehabilitation
- Correct rehabilitation is essential after an operation of this type. Rehabilitation should start as soon as possible and on the first few days you must not travel or do any strenuous or violent movements. That is why we recommend that before you go back to your country you should spent at least eight days doing rehabilitation at our Casaverde rehabilitation centre.
- This will help you to improve muscle tone and for the muscles affected by the surgery to gradually become stronger, which will reduce the risk of falling or complications.
- This will optimise mobility of the joint affected and reduce any pain and/or discomfort that may appear after the surgery.
- Improves trophism – nourishes the tissues around the operation site and encourages correct healing and closure of the surgical wound.
- Recovers motor skills, giving the patient help, guidance and re-educating them to adopt walking patterns that will soon have them on the road to recovery.



